Most visitors to this site will likely have heard the news already, but I have pancreatic cancer that has spread to my liver.
I don’t smoke, I don’t drink, and there’s not really a history of pancreatic or liver cancer in my family—so this was completely unexpected. Since two great-grandmothers reached their 100th year and all grandparents died in their nineties, I actually thought I’d attend at least the 2060 World’s Fair. (If they still have them then.)
We also now know why PC is called the “silent disease,” because I basically had no indication this was taking hold of my insides. It started little less than a month ago with an itch.
An itch that wouldn’t stop. That eventually spread all over my body. It wasn’t awful itching—I could usually ignore it during the day. But there didn’t seem to be a cause. I’ve had dry skin, and bad cases of poison ivy, but this didn’t seem to be either. I tried various lotions and an antihistamine and waited for it to go away.
After a week, though, the itching was affecting my sleep. I found a highly rated dermatologist on Yelp and got their earliest appointment—a week away.
By the end of this second week of itching, I was getting a number of tiny sores. But the dermatologist agreed with me that they were the result, not the cause, of the itch. He also did not see any immediate cause for the itch and prescribed an antihistamine.
But he did notice that the whites of my eyes looked a reddish-yellow. Partly out of concern for that, and partly because hepatitis can cause itching, he recommended some blood tests. I promptly went across the street and had blood drawn.
The next day was Friday, and just as I was leaving the office I got a call from the dermatologist. He wanted me to check in to a hospital, as my bilirubin and glucose numbers were off the chart.
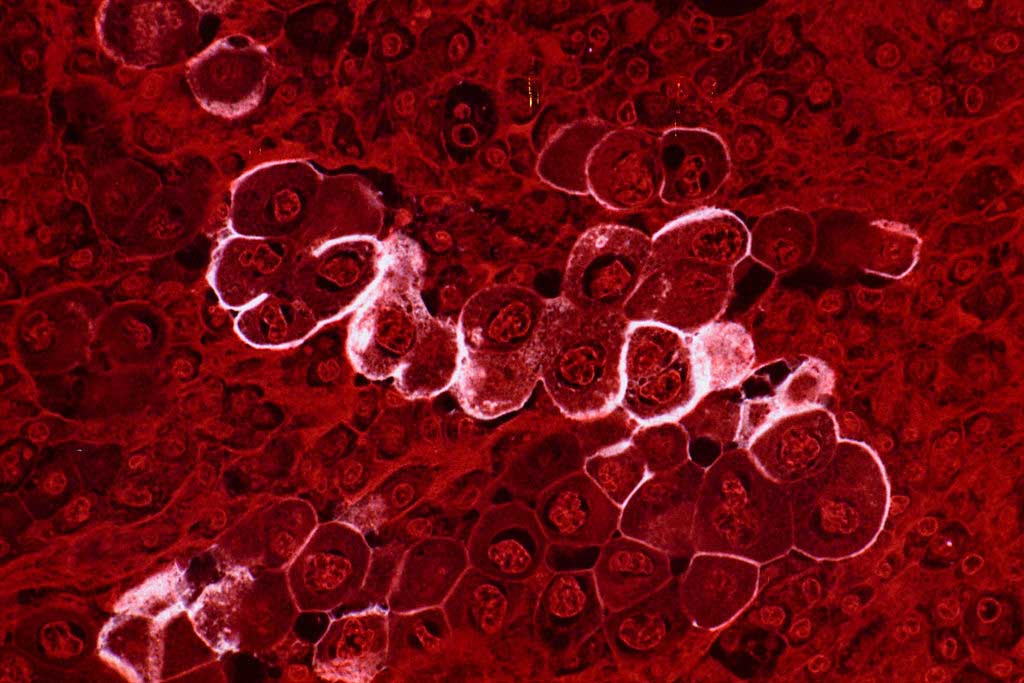
Sometime after midnight in the ER, a sonogram followed by a CAT scan finally pinpointed the cause of the itch: buildup of bile in the bloodstream and skin, caused by a growth on the pancreas blocking the bile duct. There also seemed to be some suspicious liver spots.
Things got very serious, very fast. Except that in hospitals, as in all large organizations, “very fast” had to wait on procedure. My gastroenterologist wanted to perform an ultrasound endoscopy, which would be able to get a biopsy of the growth—but over the weekend only regular endoscopies were performed. Nonetheless, I had the regular endoscopy Saturday morning to take a closer look and open up the bile duct with a stent.
Turns out, the difference in endoscopy had no practical effect—the ultrasound endoscopy on Monday grabbed a sample from the growth, but oncologists were unable to declare it cancerous with certainty. Meanwhile, the bile was still not draining, so the jaundice and itchiness (remember the itching?) continued.
Tuesday I had an MRI, which teased some hope by suggesting that the liver spots were merely enlarged blood vessels and the growth was smaller than originally thought (1.2cm instead of 3cm).
Even with the MRI, however, the radiologists still could not determine with certainty that the growth was cancerous. My gastroenterologist wrestled with how to continue—he wanted to perform a biopsy to get that certainty, but I still had no itch relief and scheduling the biopsy would be at least another day. He consulted with colleagues, and everyone’s gut instinct (so to speak) was that the growth was indeed cancer.
So instead of taking another day for a biopsy, he instead suggested immediate surgery to remove both the growth and the gall bladder (to clear up the bile issue). After nearly a week of sitting around the hospital, this sounded like a much more preferable course of action. Aggressive cancer requires aggressive treatment, and cancers of the pancreas and liver are apparently among the most aggressive.
Not that we understood how much this surgery entailed. The “Whipple procedure” or pancreaticoduodenectomy (and doesn’t the length of the name say something about the complexity of the procedure?) is known as the most complicated abdominal surgery around. It consists of
the removal of the head of the pancreas, the duodenum including the duodenal papilla or ampulla of Vater, the proximal jejunum, gallbladder, and often the distal stomach.
Wikipedia also specifically states that it “is performed to treat cancerous tumors of the head of the pancreas,” so you can see why it was of interest. To save time, my gastroenterologist recommended direct transfer to George Washington University Hospital, one of the top local institutions for this surgery.
Of course, it took two more days to actually accomplish that speedy transfer. And the GWUH radiologists wanted to examine all my scans themselves before signing off on this huge procedure.
Meanwhile, we learned that the success rate (no return of the cancer within 5 years) was only about 50%. There was also still some suspicion of those liver spots—although the GWUH radiologists concurred that they didn’t seem to be cancerous, there was no certainty. And there could be smaller spots the MRI missed. This was important because if the growth was cancerous AND had spread to the liver, there was no point in removing all those pieces of organs.
I was wheeled into the OR early Saturday morning, nine days after meeting the dermatologist, for what was expected to be an 8-hour surgery. I was wheeled out after 3 hours because the cancer had in fact spread to my liver.
This was an extremely hard day for my wife and parents. (I was still out of things on the remnants of general anesthesia.) Up to that moment, there was an astronomically small chance the growth on the pancreas wasn’t even cancer! Instead, it was too late to cut out the tumor.
In case you’re wondering why it took three hours, it’s because they still removed the gall bladder in an effort to quell my jaundice and itching. (Remember the itching?)
It’s very late Sunday night as I write this, and it’s just been a day of breath-catching. Of supporting one another, spreading the word to family and friends, and of hearing in turn all their wishes of care and support. Thank you all.
As long as this post was, it’s only covered the basic facts. I’ll follow up at some point with a more introspective commentary.
we love you elliot
Elliot when we heard about your condition me and jeannie sat down and I cried. Gary asked what was wrong and I told him and he just got silent he said grant I am sorry to hear that new and he asked if I was ok I just told him that I was just numb and in disbelief. I know we are not very close but I love you with all my heart and soul and we are praying for you. Since hearing about it I have just been really quiet and pretty much to myself. I have things going on with my health but you are always on my mind. Just take care spend alot of time with anne and the boys and just keep us posted on how you feel
Take care
We love you
Me jeannie and gary
Thanks Stefon! I love you too
Thanks Stefon! I love you too cousin. I hope we can both get past these health issues and get on with life. In the meantime, as you say, family is so important. I'm glad you have Jeannie and Gary there for you as I have Anne and the boys.
Love to all,
etg
Carolyn, thank you so much
Carolyn, thank you so much for your beautiful, thoughtful, and caring response. Nothing was offensive in the least, and in fact it sounds like we have remarkably similar views on many aspects of life. I don’t know yet if I will survive as you have, but you are a wonderful role model.
Your comment did post to the site, but you didn’t see it because I have to approve all comments. (Prevents spam messages.) I will approve it immediately, because I want other visitors to benefit from your hard-earned insights as well.
Sorry I haven’t seen you, Neil, Meredith, or Michael for a while but my parents have been keeping us in the loop. Sounds like you have much to be proud of in your children.
Thanks again for all the support—not just for me, but (even more importantly to me) for my parents. May the road rise up to meet you, as the Irish say.
etg
Thinking of you.
Hi Elliot,
Thank you for sharing the details of the dire illness you are facing.
To some degree I have shared your position as a cancer patient (two different cancers, twenty years apart) and the experiences of discovery, testing and waiting. A lot of people have called me courageous and such things. The fact is, in my experience, you have no choice but to hold fast to your best judgement for managing yourself and trying to help your loved ones.
At the same time, I have had the experience of looking over the abyss and facing up to the end of my life. I continue to do that with every 3 month CAT scan that comes as a reminder of my situation in life. I know that everyone who lives is in the same ultimate position but denial and presumed health keeps it at bay.
From my bout with pancreatitis (not cancer), I am glad to hear you seem to be relatively comfortable. I hope you will avoid any such pain and do all you can to keep it at bay. I sympathize with your itch. It was the most annoying symptom of my recent radiation burns.
I am as atheistic as a thinking person can be. My ultra agnosticism came on much as you have described for yourself -over time and with education and thought. I had a French professor in my freshman year of college who gave me the greatest solace I had ever received in coping with my inability to accept the religious beliefs of every adult I knew in my youth in southern Virginia.
She, in her 60's I think, said, "I've never been able to believe it either, but if there is a God, unless he's worse that Hitler, Mussolini and the rest rolled together, he'll do nothing but welcome me with open arms." While admittedly anthropomorphic for some tastes, that comment helped me for the very first time and I still find her words helpful.
Your concept of a moral life certainly meets with my full agreement and I thank you for putting it so succinctly.
As a mother of two youngish adults, I cannot imagine the pain of losing either one of them and I know your parents are suffering. Your insistence that they keep on with their normal lives will be of great help to them. They are going to do everything you ask because of their love for you, as you well know.
Once, when I had an acoustic neuroma (not cancerous) I faced a 10 hour surgery that required a brain surgeon to open my skull, drain the liquid from around my brain and move it into position to allow the removal of the tumor that had wrapped around my acoustic, vestibular and facial nerves and was pressing on my brain stem. I was assured that the surgery would not put my life in danger, but with all that would be going on, my common sense said I had to prepare for a situation where things could go wrong.
I spent time alone isolating my fear and deciding just what I was afraid of in fearing death. I concluded it was the state of nothingness. I was afraid of nothing. (Have you read Julian Barnes?) It seemed like a word trick, yet there was a kernel of truth in it. I was afraid of nothing. It was a kind of relief and I concluded that if I should live, I would awake with the thought…"ahh…more life.”And that's exactly what happened.
But prior to that I realized I had two choices for the time leading up to my surgery, a period of about two weeks. I could terrify myself and suffer, or I could have the best time possible. Meredith and Michael came to town the last week before surgery and we did just that.
We had a wonderful, cheerful week. When some fear and sadness was expressed by Meredith, I insisted she join me in enjoying the moment and she came through. I slept soundly each night and on the morning of surgery I was cheerful. Meredith's boyfriend had a flute and piped me off to surgery, delightfully high on some preoperative drugs.
I awoke to "ahh life…” followed almost instantly by a hell of side effects. But over the days as I got better and got back to my more normal self, I came to regard and still regard that week before the surgery as the greatest accomplishment of my life. Something between me and me. I could be my own best friend. And I did something good for my family and friends as well.
I share this with you because I think I understand something of what you may be feeling. Being strong for yourself and others is a great accomplishment and a great gift to yourself and others. You can give your sons one of life's greatest lessons and your loved ones the greatest possible comfort. Also, you will go not as a victim but a man whose strength and power prevailed.
Kirk Vonnegut said "Life is a terrible thing to do to a person." I would add that just being here for 10 or 100 years, makes you a winner of the greatest lottery in the cosmos. Congratulations on all you have done and all that is still in store for the unknown space in time to come. We are all in this together.
I hope my comments do not offend you. They come from my heart and are meant to be helpful to you. I find it is difficult for people to speak about such things but I think communication is everything so I offer my words.
These days I keep up with you through your parents and now this site I’ve just learned about. I would like to tell you that I admire the choices you have made in life and I wish you all the best in the days to come.
You may be sure that Neil and I will do all we can to bring your parents comfort and enjoyment in the future.
With love,
Carolyn
jonsimons@westat.com
Elliot,
Dan shared this link with me, and I want to offer my support. My mother had pancreatic cancer many years ago, so I know what you mean by the silent disease.
There will be both good days and bad days ahead. I'd like to be part of your support team from work.
Positive thoughts.
Jon
Thanks, Jon!
You most certainly are part of the support team. Thanks so much for sharing your message. I don't know many people who get to work with as good a team as I do at Westat.